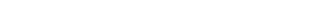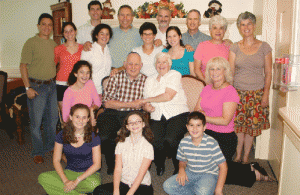Coming Out and Pushing Back Against Alzheimer’s, Part Two by Joan Brunwasser & Elaine Reisman
October 30, 2015Guest Bloggers Joan Brunwasser & Elaine Reisman
February 10, 2014
You can read more about Elaine and Bernie’s story here on The Genius of Caring site.
Welcome back for the conclusion of my interview with Elaine S. Reisman. Elaine’s husband Bernie suffered from Alzheimer’s Disease for the last sixteen years of his life.
Before we broke, we were going to talk about how Alzheimer’s affected your life as a couple, Elaine. What can you tell us?
ESR: We continued to have an active social life, entertaining and having lots of company for dinners and visiting. Old friends invited us out but it was more difficult for friends who knew us before the dementia. This was not the man they knew. So, it was easier to socialize with new friends whom we met through support group and day care, because they knew him as he was at that time.
We also still took some trips, even venturing overseas as we were accustomed to doing; however, Bernie’s constant questioning sometimes became annoying. I covered for him as much as possible, but then would explain (out of his hearing) that he had Alzheimer’s.
JB: In what other ways did the illness impact your lives?
ESR: Although we continued to travel, the trips were stressful for me. But I was glad that we could still do them as we enjoyed traveling.
The problem with traveling was that if he had to go to the men’s room, I had to wait outside and hope that all was well. Once, while I was sitting with our luggage, Bernie came out and headed in the wrong direction. I had to abandon our luggage and run after him. I wondered then whether it was really worth it to travel.
One day, we were in downtown Boston waiting for the T. When the train arrived, I thought Bernie was with me, but he had evidently gotten onto a car by himself. Before I knew it, the train was moving on. I quickly went to the dispatcher who radioed ahead and arranged for someone to take him off the train until I could get on the next one. When I caught up with him, he was sitting and having a great conversation with the two agents who were sitting with him. No need to mention how I felt!
Probably the most difficult challenge occurred when Bernie had to stop driving.
JB: Tell us more about this, please.
ESR: When it became clear that he should no longer be driving, that was a BIG one. He was assessed and, because he still seemed OK, he was told that he could still drive short distances. That truly posed a problem. Fortunately, one of our two cars conked out, so I could concoct lots of excuses. “We have to go on the highway and you know the doctor told you not to drive on the highway” and other such ruses. One day, he was very insistent so I got the doctor on the phone to convince him. From then on, I kept a written note from the doctor and pulled it out when he insisted on driving. That seemed to satisfy him.
Once someone can no longer drive, the burden on the caregiver is even greater. I realized that I was delaying having Bernie tested because I knew that once he wasn’t driving, that would further complicate my life. We supplemented with car services available in our area, but you can’t minimize the psychological implications, particularly for men who are no longer in the driver’s seat. Needing to stop driving means a loss of independence and control. Driving is macho!
As the challenges became greater, it was clear that the nature of my role was irrevocably shifting from wife to caregiver.
Which leads to the topic of intimacy.
JB: I was wondering about that.
ESR: Our marriage relationship had always been very good for both of us. But now, it became difficult for me to be responsive. Romance is difficult to maintain when you have to get up in the middle of the night and walk through puddles of urine to check on your loved one who may be sleeping on the floor in the living room. Or, when you are doing the laundry and it is necessary to deal with soiled underpants. One way we kept a spark going was when we took walks together. We always held hands, even before the illness, but now this contact had a special quality to it. We walked along very close to each other, holding hands, and I would feel a sense of closeness. This was good and bad–it sometimes gave me false hope that we could return to the old days, even though I knew that was not to be.
I felt like I was being teased. He is here, but he isn’t.
Then, came the letting go.
JB: What do you mean by that?
ESR: The children were after me to place him. I knew that was in the picture, but it was difficult to face. There is an element of “no one can care for him like I can”. However, it was clear that I did not like having the help in the house–even though it was only for a few nights a week. Also, I had to fire one woman. She was too rigid and one morning I came down and Bernie was in tears. That did it. Although some of the aides were wonderful, I did not want anyone else taking care of him.
However, it became clear that the time had come and the children and I investigated places, finding one that was very convenient for visiting and seemed to be appropriate.
JB: How did that go?
ESR: It was a nightmare! Bernie still needed a lot of activity and was not about to just sit and watch TV. Although the facility we chose met all legal requirements, the supervision was inadequate to meet the needs of a more active resident. He urinated in the plants, wandered into rooms, and got into bed with others. Bernie still retained the image of himself as a facilitator.
So, he would often try to get the other residents to come to a “meeting’. He went from person to person and tried to get them up and out of their chairs so they could come with him. This was a safety issue for him and the others, who could have fallen and hurt themselves. Rather than distracting him by making a game out of this, the staff saw Bernie’s actions as disruptive and were confrontational, which made things worse.
The staff viewed Bernie’s behaviors as agitation and the consulting psychiatrist recommended a low dose of anti-psychotic medication, which actually made him worse. One time, according to their report, Bernie kicked an aide who was trying to get him ready in the morning. This was so not like him that I have to assume he was greatly frustrated. At times when I was in a room full of residents, staff was nowhere to be seen. In this incident, I assumed that the aide was rushing him to get dressed because of the pressure of her other responsibilities.
The nightmare got worse when we were told that we would have to hire a full-time companion or have Bernie evaluated. We chose the latter and he was placed at a local psychiatric hospital for evaluation. They continued to administer anti-psychotic medication which caused him to hallucinate and I wondered how they could evaluate him without trying to engage him. It looked to me as though they just stood around observing him as he undressed in the halls. They then put him into a one-piece garment he could not undo and continued to try different medications.
Visiting him was horrible!!! It was a ward with psychiatric patients exhibiting unpleasant behaviors. I took him out and – don’t tell – I drove him around off campus. When it was finally agreed that he should move on, it was difficult to find an appropriate setting. They were crushing his pills, so that limited facilities to a nursing home. He was still in good enough shape that he needed activity more than medical care.
With the superb support of the Alzheimer’s Association, we finally located an assisted living program for Alzheimer’s Disease with a philosophy of trying behavioral and environmental accommodations for people with dementia. This proved to be a most satisfactory arrangement for about two years.
Here, Bernie also tried to organize “meetings’. But, there was more of an effort to redirect him as he tried to get people up and out of their chairs or wheelchairs. In thinking over this nightmare, I still carry some guilt. I feel as though I should have been more assertive about the medication. Since then, researchers and professionals in the field have questioned the use of anti-psychotic medication for dementia.
JB: Were there other situations where Bernie was still alert and tuned in, despite his dementia?
ESR: Before Bernie was placed in 24 hour care, he was invited to testify before the US Senate Committee hearing advocating for more research and for higher standards of training for aides for Alzheimer’s patients. As we sat there waiting for his chance to speak, I was apprehensive about whether he would be able to speak coherently. He astonished the audience who were well aware that he was an Alzheimer’s patient when he stood up and addressed the packed room as though he were still a professor delivering a lecture.
Once Bernie was in 24 hour care, there were still instances of his being with it in spite of the dementia. We were all moved by his participation at our granddaughter, Lianna’s pre-Bat Mitzvah.
Whenever he was with Lianna, she found a way to engage him: she would involve him in an exercise routine or some games. She said she did not want to be Bat Mitzvah without Bernie’s presence and it was clear that he could not travel to Baltimore. So, a few months before the actual Bat Mitzvah, we arranged with the facility to use the living room for a pre-Bat Mitzvah ceremony, borrowing a Torah, and all 18 of the immediate family gathered for the service, which she and her family conducted. Although Bernie could not recognize a single one of us, his whole demeanor including the expression on his face nevertheless indicated that he clearly knew that this was an important event. At an appropriate point in the ceremony, he spontaneously stood up and spoke about the family with emotion and clarity, as though it were the old days, BA (Before Alzheimer’s).
Family was very much involved in all decisions and their support of whatever I did was helpful. It really makes a difference when a family can agree. In support group, we heard of the angst in families where there was disagreement about the care of the patient and often about related financial matters.
Fortunately, early on in support group, I had learned about getting involved at the VA. With that contact established early on in the disease, we knew that when he needed nursing care, he had a place to go.
Bernie thrived at the assisted living facility. However, after two years, his condition worsened. He became less steady on his feet and less able to engage in activities. He also caused major flooding damage when he turned on water in the laundry room and left it running. It was determined that he was now ready for more medical care. At that point, we moved him to the VA. Again, personnel at the Alzheimer’s Association were most helpful, practically and emotionally, in the transition.
The personnel and the care at the VA were excellent, but it is not pleasant to visit any nursing home. Bernie maintained his pleasant appearance in spite of the dementia. He also still maintained a pleasant demeanor and the aides and nurses appreciated his expressions of appreciation although by now, it was mostly a smile or maybe a word or two. He was no longer able to walk and needed to be fed.
Robin, Sharon, Joel and Eric with Bernie
Local family visited him and the out-of-towners kept in touch by phone, although those were really just one-way conversations. They came in to see him as much as possible. Having another person present made the visit easier and we sometimes had family visits at the VA. We soon got to know family members of other patients and that was also a help.
By then, Bernie’s responses were minimal but he did light up when the familiar aides came in. Sometimes we would sing to him or tell jokes among ourselves and occasionally talking about something familiar to him, he might repeat a word.
I just remembered another ceremony we had. When we first placed Bernie in 24 hour care, we put a mezuzah on the door of his room. Then, we went back home and had time together, our four kids and me. Joel had written a beautiful poem and we all reminisced. It helped a great deal with the transition. Sharon had also downloaded my emails to the family and put them in a notebook as a way of supporting the decision by verifying all that we had done to care for him, short of placement.
Something that threw me: the VA has a family picnic each year. We were sitting together where the dance band was playing and a few people were “dancing’. I looked at him and saw that he was crying–not just tears coming down–really crying. So I hugged him and tried to reassure him and then got an ice cream to feed him. My read on it was that the music reached him. We used to go dancing. Robin said that when she took him to one of the music sessions, he had the same reaction.
When they moved Bernie to a private room for the final hours, we arranged for the rabbi to come. Local family was there and we hooked up by speaker phone to those not able to come. We each spoke to Bernie, who by that time was totally out of it. This proved to be a very important part of the good-bye process.
Now, I look back at all of this with a feeling that we all did the best that we could and tried to maintain some quality of life for him and for our relationship with him as the illness progressed. In many ways, I feel very proud of myself for finding ways to cope and afford him as good a quality of life as I could, under the circumstances. I feel good about being helpful to others who are going through similar situations.
I still regret having been impatient, not being more forceful about the medication, and the poor choice of the first facility. And I’m grateful for family, friends and the Alzheimer’s Association for their support.
JB: What about now, Elaine? What have you been doing with yourself? How do you keep busy?
ESR: When Bernie went into 24 hour care, I sold the house and moved into a continuing care community. This has proved to be an excellent choice for me. I swim every morning. I call it my hydrotherapy as I often wake up feeling crumby and know that my spirits will rise once I have my swim. I also play bridge, read and take walks.
I continue to offer courses at BOLLI, a life long learning program that Bernie started at Brandeis University after he retired ( and about five years into the illness). These courses afford me the opportunity to explore subjects of interest and boost my ego because of the positive response.
Our children continue to be attentive and involve me in social activities and I make sure to schedule visits with friends.
This picture was taken in August, 2013. I was at Joel and Debby’s for brunch to honor my 85th birthday. The other three children and their spouses and families were unable to attend this event, so each family was represented at the brunch with a food contribution: brownies from Baltimore, the salad from Newton, and a food basket from Hartford.
Since we could not get the whole family together for any single event, they planned a variety of activities involving every member of the family. I had a total of eight different celebrations: canoeing, playing games with my grandchildren, a week-end in the Berkshires with Sharon and Robin, a week-end in Baltimore with Eric and family where we played a game created by daughter-in law Sheryl that celebrated my life, museum excursions, visits to my apartment and receiving cards and calls. Each member of the family was involved in some way to honor me.
My newest career is as a producer/director of full length plays. Residents here, many in their nineties, participate in the reading/acting productions and the response from them and the audiences is most fulfilling for me.
It’s safe and friendly here, but I truly miss my best friend.
JB: I bet. Thanks so much for talking with me and sharing some very private aspects of your life with our OpEdNews readers, Elaine.
ESR: Thank you, Joan. I’m grateful to you for affording me this opportunity to reflect.
JB: Thanks again for talking with me, Elaine. This has given me a chance to reflect too. Bernie has been an important part of my life since he mentored me during my grad school days at Brandeis.